Rh and ABO Incompatibility
Rh & ABO Blood Incompatibility
The mother’s body/placenta/nourishes fetus while the baby is in utero. Sometimes small amounts of blood pass through the placental barrier to the mother.

In most cases, the mother’s blood is compatible with the baby’s blood. However, sometimes a disorder called Rh incompatibility develops. This increases the chance that the fetus will develop life-altering and life-threatening conditions.
Doctors, nurses, midwives, and medical facilities must diagnose and treat the mother and baby when they suspect RH incompatibility. Without proper diagnosis and treatment, the medical providers will have committed medical malpractice. Meanwhile, the mother may find that her newborn baby has sustained irreversible brain trauma.

To understand how babies can be hurt by their mother’s blood, we first must understand more about the Rh factor.
What is Rh Negative Blood?
“Rh” refers to the rhesus factor, an antigen found on the surface of some people’s red blood cells. About 85% of humans have Rh-positive blood. Generally, being Rh-negative is not a problem except for pregnant women and their babies.
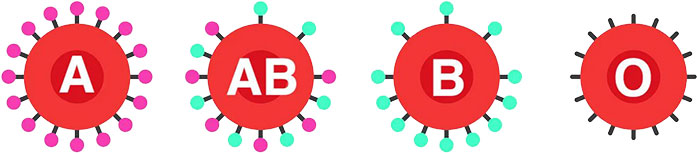
Everyone has a blood type – either A, B, AB, or O. But each type is also split into different categories based on several factors, including whether Rh protein is present. A person’s blood type might include “positive” or “negative” to indicate their Rh status. For example, someone with A positive blood has Rh while someone with A negative blood does not.
Statistically, about 15% of caucasians are Rh-negative, 5-8% of African Americans, and only 1-2% of Asians and Native Americans.
What is Rh Incompatibility?
Parents pass genes to their offspring that determine their blood types. A baby’s blood type is determined by its parents’ blood types. For example, if the mother is A and the father is O, the baby’s blood type will be either A or O.
The general blood type is not what causes Rh incompatibility. The problem occurs when the mother is Rh-negative and the baby is Rh-positive.
How Can A Rh-Negative Expectant Mother Have A Rh-Positive Baby?

- Mother is Rh-positive. There’s no risk for Rh incompatibility.
- Mother is Rh-negative and has Rh antibodies in her blood. Her baby is at risk for Rh incompatibility.
- Mother is Rh-negative with no antibodies. Father is Rh-negative. The baby has zero chance of having Rh-positive blood
- Mother is Rh-negative. Father is Rh-positive. Their baby has at least a 50 percent chance of having Rh-positive blood. There’s a high risk of Rh incompatibility, especially if this is not the mother’s first pregnancy.
- Mother is Rh-negative. Father is Rh-positive or unavailable for testing. The doctor should do tests like an amniocentesis to learn the baby’s status.
Expectant mothers and their babies usually do not share blood, but small amounts of blood sometimes transfer from baby to mother. When this happens, the mother’s body views blood from an Rh-positive baby as a foreign substance. An immune system kicks in and creates antibodies to combat that substance.
When this occurs, the mother’s antibodies can cross the placental barrier and enter the baby’s bloodstream. Because of the Rh incompatibility, the antibodies then begin to attack the baby’s red blood cells, damaging and sometimes destroying them.

First Pregnancy vs. Subsequent Pregnancies
Rh incompatibility is usually not a problem in an Rh-negative woman’s first pregnancy. However, her doctors should still test for antibodies at her first prenatal visit because there are several reasons a mother could have Rh antibodies:
- Prior pregnancies that did not end in a live birth including miscarriages, ectopic pregnancy, induced abortions, stillbirths, evacuation of molar pregnancies.
- Testing during pregnancy, including chorionic villus sampling (CVS) and amniocentesis
- Delivery of an Rh-positive baby
- Complications during pregnancy and labor, including antepartum hemorrhage, external cephalic version (manually turning the baby from breech to normal presentation, manual removal of placenta, and placental abruption
- Abdominal trauma while pregnant
- Blood transfusions, bone marrow transplants, and stem cell therapies
- Injections that could contain traces of Rh-positive blood cells

Even women with no prior pregnancies should be tested for Rh antibodies as early as possible. Doctors who know that Rh incompatibility issues are present can immediately begin to consider ways to eliminate or minimize damage to the baby.
If a obstetrician or maternal fetal medicine specialist fails to conduct these prenatal tests it may constitute medical malpractice because the opportunity to treat this condition prior to delivery will be missed.
What Is ABO Incompatibility?
A baby’s blood type is determined by genes passed down from the mother and father. For example, a mother is type O, and the father is type A. Their baby’s blood type will be either A or O.

As with Rh incompatibility, problems can arise when the mother’s blood type contrasts with her baby’s. However, this condition only occurs when the mother is blood type O. For example, incompatibility occurs if the mother is type O, and the baby is type A, B, or AB. If the baby is also type O, then the mother’s body should not produce antibodies if their blood intermingles.
ABO incompatibility generally is not as severe as Rh incompatibility. The most common problem that arises is mild jaundice. Extra feedings can help clear excess bilirubin from the baby’s body. Doctors can treat the baby with phototherapy and fiber optic blankets if jaundice is more severe. In rare cases, the baby may need a blood exchange transfusion or a transfusion of additional red blood cells.
At prenatal visits, doctors should screen for ABO blood groups as well as Rh antibodies. Knowing about incompatibility before labor and delivery allows medical professionals to be prepared to handle any complications.

Identifying and Treating Rh Incompatibility in the Mother
Doctors who treat a pregnant woman should conduct several tests as soon as possible, usually at her first prenatal visit. It’s crucial to determine:
- Blood type: If the mother is O, the doctor can watch for ABO incompatibility.
- Rh status: If the mother is Rh-positive, then there’s no risk of incompatibility. However, further testing and monitoring are needed if she is Rh-negative.
- Rh antibodies: Doctors can and should screen for Rh antibodies using blood tests, including direct and indirect Coombs tests. Even in an Rh-negative woman's first pregnancy, the potential risk is too significant to ignore.

A substance called Rh immune globulin is given to mothers with Rh antibodies. Rh immune globulin, also called RhIg or Rhogam, contains Rh antibodies that attach to Rh-positive blood cells. The mother’s immune system then stops creating antibodies that attack the baby’s blood.
The timing of the RhIg injection depends on the mother’s medical history and her antibody status:
- First pregnancy, no antibodies. In a first pregnancy where the mother has no Rh antibodies, the doctor can treat potential Rh incompatibility after the baby is born. However, additional screenings should be done throughout the pregnancy to ensure that the antibody status hasn’t changed.
- First pregnancy, with antibodies. Doctors and other medical professionals caring for the mother should increase monitoring of mother and baby. An Rh immune globulin injection should be given at 28 weeks, within 72 hours before delivery, and after delivering the baby. Mothers who experience any events during pregnancy that could cause Rh incompatibility – like abdominal trauma –may need additional treatment.
- Subsequent pregnancies. Once the mother has Rh antibodies, Rh incompatibility will likely complicate future pregnancies. The mother’s physician, nurse, or midwife should increase screenings and monitor the mother and baby more closely.
A pregnant woman with Rh incompatibility may not exhibit any signs. However, her baby could be in danger.
Rh Incompatibility’s Effect on Babies

Babies of Rh-negative mothers typically become anemic because their red blood cells are being destroyed faster than the body can replace them. This condition is called hemolytic anemia or hemolytic disease of the newborn (HDN).
The long and short term effects to the infant depend on the severity of the anemia:
- Mild: Sometimes the fetus can tolerate the Rh incompatibility without any serious problems. Their anemia does not cause any serious problems. As a newborn, they will probably be jaundiced. Both the anemia and jaundice may resolve without treatment and without permanent damage to the baby.
- Moderate: Bilirubin levels may stay pretty low before the baby is delivered. However, those levels can dramatically increase within 24 hours after delivery. The baby’s medical providers must diagnose and treat high bilirubin levels before permanent brain damage occurs.
- Severe: The fetus’s liver and other organs work harder to make up for the reduction in red blood cells. The organs then may become enlarged (hepatosplenomegaly). Liver dysfunction can occur, and immature blood cells enter the baby’s bloodstream. The baby could develop hydrops fetalis, which is usually fatal.
Other severe conditions can develop in a fetus or newborn due to Rh incompatibility:

- Oxygen deprivation: Since red blood cells carry oxygen throughout the body, Rh incompatibility can cause oxygen deprivation called hypoxic-ischemic encephalopathy (HIE) that damages the baby’s organs and brain. Brain injuries can cause lifelong problems, including cerebral palsy.
- Heart Failure: The baby’s heart will be pumping harder than average, which can lead to heart failure. Hydrops fetalis due to heart failure cause fluid to accumulate and fetal tissue to swell. This condition is usually fatal to fetuses and newborn babies.
- Neonatal Jaundice: Rh incompatibility can cause newborns to develop severe jaundice (hyperbilirubinemia) caused by high bilirubin levels in the baby’s blood. Kernicterus can develop, which is a type of brain damage that can cause hearing loss, cerebral palsy, and more.
Rh incompatibility can be fatal to the fetus or neonate in severe cases. The infant may also have permanent brain injuries that require medication and treatments for the rest of their lives.
Identifying and Treating Rh Incompatibility in the Baby

Usually, doctors will first identify the mother as Rh-negative and having antibodies in her blood. Identifying Rh incompatibility in a fetus may be more difficult, but it is crucial for the baby’s health.
Doctors might only suspect a compatibility issue. However, the following tests can confirm whether the fetus is suffering from hemolytic anemia or other conditions brought on by Rh incompatibility:
- Test the baby’s blood velocity: Using Doppler ultrasonography, the doctor can check the baby’s middle cerebral artery. This non-invasive method of testing measures the peak systolic velocity of the baby’s bloodstream. The baby’s heart may be working harder because of hemolytic anemia. Blood that is flowing faster than normal can indicate the baby has hemolytic anemia.
- Test Rh status: Amniotic fluid or fetal cells from the umbilical cord can indicate whether the fetus is Rh-positive or negative. Doctors will then know whether Rh incompatibility is an issue.
- Test bilirubin levels: After the baby is born, doctors must closely watch the amount of bilirubin in the baby’s blood. High levels of bilirubin (hyperbilirubinemia) can cause brain damage.
Mild levels of Rh incompatibility may resolve on their own, but treatment is usually necessary to protect the baby. Before the baby is born, doctors may inject the mother with Rhogam, an Rh immune globulin, to reduce her body’s immune response.
After the baby is born, doctors address high bilirubin levels with phototherapy, blood transfusions, or blood exchange transfusions.
Preventing Rh Incompatibility and Its Complications
Doctors cannot prevent an Rh-negative mother from having an Rh-positive baby. However, they can address the way the mother’s body reacts, especially to subsequent pregnancies.

Testing, screening, and monitoring the mother will tell the doctor if Rh incompatibility is a complication. They can then develop treatment plans to protect the baby.
Mothers also need to have Rh immune globulin injections for subsequent pregnancies.
Doctors and other medical professionals must be aware of the mother’s Rh status to reduce complications for the baby. Failing to test the mother and identify Rh incompatibility early can lead to brain damage, hyperbilirubinemia, hypoxic-ischemic encephalopathy, cerebral palsy, or death.

Was Your Child Harmed Because Doctors Failed to Treat or Manage Rh or ABO Incompatibility?
The parents of children who suffered birth injuries often want answers. They want to know what happened to harm their child’s brain. Was it preventable?
Our dedicated birth injury lawyers want to help you find those answers.
We diligently investigate the facts and hold responsible parties accountable by pursuing medical malpractice claims against them. The compensation our clients receive helps them pay for their child’s current and future medical treatment, assistive technology and equipment, and the other expenses associated with caring for a child with brain injuries, seizure disorders, and cerebral palsy.
Sometimes families are afraid to talk to lawyers about their child’s case. Others may simply feel overwhelmed by their circumstances and unable to participate in a lawsuit involving their child’s birth injury.
Why Should You Talk with the Knowledgeable Attorneys at Miller Weisbrod Olesky?

The only way to find out if you have a birth injury case is to talk to an attorney who understands birth injury.
At Miller Weisbrod, a team of committed professionals uses our detailed case review process to assess your potential claim. They start by learning more about you and your child. Then we gather medical records to determine what happened before, during, and after your delivery. We call in skilled medical experts who review your records and let us know if they think medical errors could have caused your child’s injuries.
If we feel medical malpractice was present, we meet with you to discuss how you can receive compensation from the medical professionals who made the errors.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment when you do.
Contact Miller Weisbrod Olesky
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034