Vasa Previa
Vasa Previa in Pregnancy
Every expecting mother hopes for the safe and easy delivery of her newborn child. Uncaught pregnancy complications like vasa previa can put both her and her baby’s wellbeing at risk during birth.
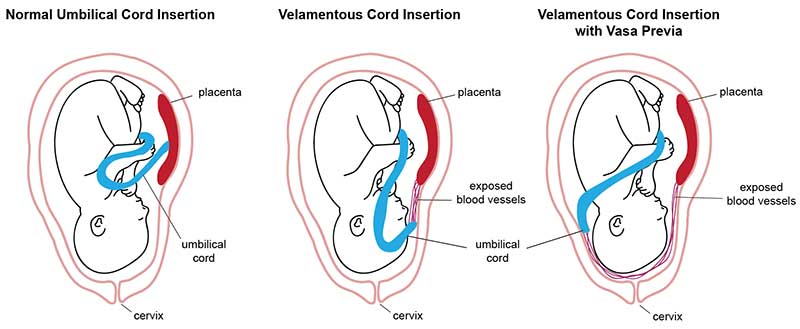
Vasa previa is a complication where important umbilical cord blood vessels run across the mother’s cervical opening. The baby’s head will press against these blood vessels as they try to exit through the birth canal during labor. That puts these blood vessels (which are normally inside the umbilical cord) at high risk for compression or even rupturing.
Only around 1 in 2,500 expecting mothers will experience vasa previa each year in the United States. When doctors identify the condition during prenatal testing visits, the fetus has around a 97% chance of surviving.
However, when medical professionals miss the signs of vasa previa, they may unknowingly have the mother attempt a vaginal delivery. This puts the baby at high risk for their umbilical cord blood vessels bursting, suffering extreme blood loss, and stillbirth.
Babies who survive after umbilical cord compression and rupturing may suffer birth injuries from oxygen deprivation. Prolonged birth asphyxia can result in multiple hypoxic and ischemic brain injuries, most notably hypoxic ischemic encephalopathy (HIE).
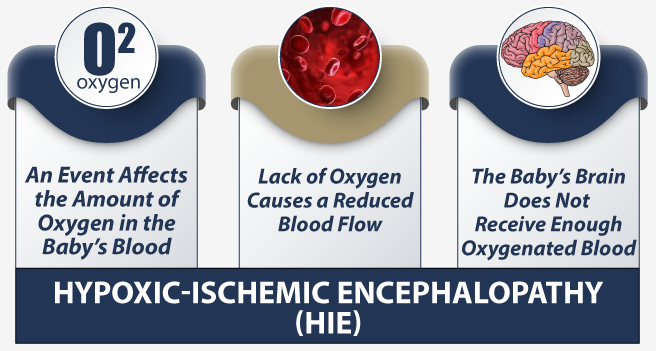
HIE is a permanent form of brain damage at birth that can cause numerous long-term health conditions. This includes seizures, vision impairments, speech impairments, feeding difficulties, paralysis, and other delayed developmental milestones. HIE is the leading cause of cerebral palsy in young children.
When healthcare professionals miss the signs of manageable complications like vasa previa, they put the baby’s life in jeopardy. If medical negligence causes a child’s preventable birth injuries or death, the family may have a viable medical malpractice claim.
Birth Injury Malpractice Attorneys
Our top rated birth injury attorneys specialize in identifying how missed umbilical cord problems can lead to severe brain injuries. If your baby suffered preventable harm from a case of mismanaged vasa previa, don’t hesitate to contact our firm. We can answer difficult legal and medical questions and investigate the facts on your behalf.
Free Legal Consultation
Birth Injury Lawyers
(888) 987-0005Our Birth Injury Lawyers are available to meet you in your home or the hospital.
Our vast network of medical experts and in-house nursing staff and nurse-attorneys gives us the edge over our competition. When we take your case, we assign you with not just an attorney but an entire medical team. This team includes attorneys, experienced nursing advocates, and seasoned medical experts.
Your team is available to assist with any day-to-day treatment you or your child may need. This includes assistance with obtaining medical records, scheduling doctors’ appointments, providing transportation, and any other problems that may arise.
We offer all of this on a contingency fee basis. This means you will not pay any fees until after we win your case and secure a settlement. Our unmatched track record of birth injury results sets us apart from other birth injury law firms.

Recent Birth Injury Settlement:
Birth Injury settlement against a hospital in which nurses and physicians failed to properly monitor the mother's blood pressure during delivery causing an HIE event resulting in neonatal seizures and cerebral palsy at birth. Our team of top-rated birth injury lawyers recovered $13,750,000 for the family to help with future medical expenses and developmental therapy.
What is Vasa Previa?
A healthy umbilical cord has two arteries and one vein which carry blood and oxygen to and from the baby. Inside the cord, a gel-like substance called Wharton’s jelly surrounds the three blood vessels for extra cushioning and protection.

Vasa previa is a pregnancy complication where the blood vessels partially develop outside of the cord. Without the protection of the umbilical cord or Wharton’s jelly, these exposed blood vessels are at high risk for rupturing.
The exposed blood vessels often rest near or in front of the mother’s cervical opening. This blocks the baby’s path for a safe vaginal delivery. As the mother’s water breaks, the baby’s head will squeeze against the exposed vessels, compressing or even bursting them.
Medical professionals should never have the mother attempt vaginal birth if they know she has vasa previa.
What Are the Three Types of Vasa Previa?
There are three main types of vasa previa. Doctors categorize each type based on whether the underlying cause was an umbilical cord complication or a placental complication.
What Is Type I Vasa Previa?
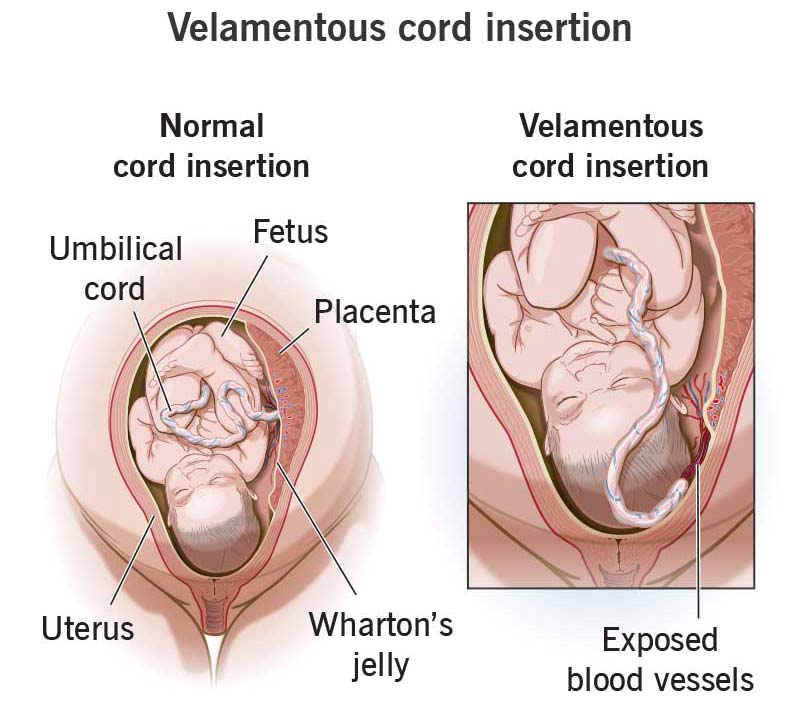
Type I Vasa Previa is usually the result of an umbilical cord problem called velamentous cord insertion. This is an abnormality where the umbilical cord blood vessels insert into the amniotic sac instead of the placenta. Velamentous cord insertion can put the unprotected umbilical cord blood vessels at risk for compressing or bursting once labor starts.
Velamentous cord insertion is the most common cause of vasa previa.
What Is Type II Vasa Previa?
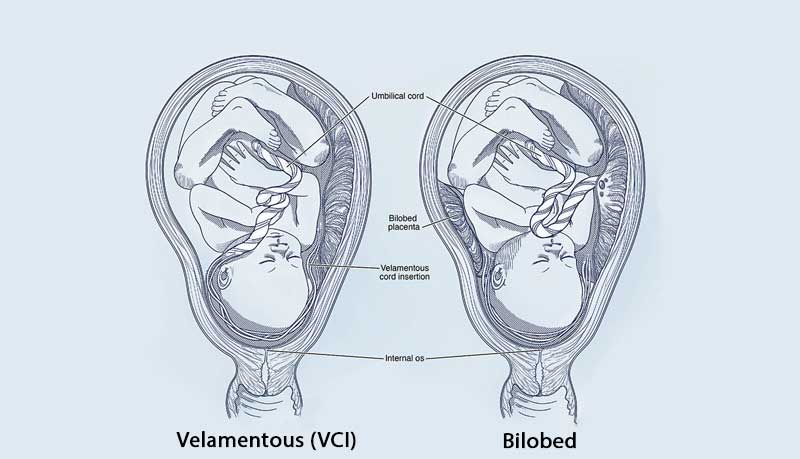
Type II Vasa Previa occurs when the mother’s placenta has an irregular shape.
Instead of developing as one organ, the placenta sometimes splits into two or more parts called lobes. This can happen because of poor blood flow in the mother’s uterus; the placenta tends to grow in blood-rich pockets. If the mother’s uterus has an uneven concentration of blood vessels, her placenta may for unevenly and have multiple lobes.
The umbilical cord blood vessels will sometimes connect the distance between a bilobed, trilobed, or multilobed placenta. Exposed blood vessels traveling between the lobes can sometimes lie near the cervix. This can cause them to burst and bleed once labor starts.
What Is Type III Vasa Previa?
Sometimes the umbilical cord blood vessels branch across the cervical opening even without velamentous cord insertion or a multilobed placenta.
Type III Vasa Previa results from vessels that originally implant into the placenta but then shoot off into unexpected directions. The aberrant blood vessels branch off from the placenta and stretch into the fetal membranes. In some cases, these exposed vessels block the cervical opening and complicate vaginal delivery.
Type III vasa previa may occur in cases with resolving placenta previa.
Vasa Previa vs Placenta Previa
“Previa” originates from the Latin terms pre (before) and via (way). In obstetric medical contexts, previa describes some type of obstruction being “in the way” of the baby’s exit.
With vasa previa, the exposed blood vessels outside of the umbilical cord block the baby’s exit through the birth canal. But with placenta previa, the mother’s placenta organ is what blocks her cervical opening.

Placenta previa and vasa previa complicate delivery in similar ways. Both complications can cause severe hemorrhaging and increase the risk of stillbirth.
For both placenta previa and vasa previa, doctors must likely schedule a planned C-section procedure to deliver the baby.
How Common is Vasa Previa?
Vasa previa occurs in approximately 1 in every 2,500 pregnancies. The complication occurs more often in pregnancies conceived using In Vitro Fertilization (IVF). Reports suggest that vasa previa in IVF pregnancies occurs in as high as 1 in 202 births. Annually, vasa previa complicates approximately 1,830 births in the United States.
What Causes Vasa Previa?
The two leading causes of vasa previa are velamentous cord insertion and irregularly shaped placental organs.

Velamentous Cord Insertion (VCI)
VCI is an umbilical cord problem where unprotected umbilical vessels run through the amniotic sac before connecting with the placenta. Vasa previa occurs when the unprotected blood vessels pass through the amniotic sac above the cervix, blocking the baby’s exit.
Bilobed, Multilobed, or Succenturiate Placenta
Vasa previa can occur when the placenta forms into two or more separate lobes. A small accessory lobe called a succenturiate placenta may also develop in the membranes close to the main placental mass. Multiple lobes often develop because the placenta tends to seek out blood-rich areas of the uterus.
The blood vessels crossing between lobes of the placenta may end up above the cervix and cause vasa previa.
What Factors Increase the Risk for Vasa Previa?
There is no single risk factor that can determine the likelihood of vasa previa during pregnancy. However, research has revealed correlations with vasa previa and other pregnancy complications.
For example, the American Journal of Obstetrics and Gynecology estimates that 60% of women with vasa previa have placenta previa.
The following are some of the most common risk factors for Vasa Previa that doctors should be aware of:
Placenta Previa

A mother has placenta previa when her placenta lies very low and blocks all or part of the cervix. Since the umbilical cord blood vessels attach to the placenta, this means they will also lie closer to the cervix. This can increase the risk for vasa previa and make vaginal delivery unsafe.
In Vitro Fertilization
In vitro fertilization is a procedure where doctors fertilize a mother’s egg in a laboratory outside of her body. They then implant the fertilized egg into her uterus.
IVF puts a mother at a significant risk factor for Vasa Previa due to the high incidence of abnormal placentation. The higher likelihood of a bilobed or multilobed placenta increases the mother’s risk for type II vasa previa.
Twin Pregnancy or Multiple Gestation

Vasa previa occurs more frequently in twin or multiple pregnancies because the prevalence of pregnancy complications and abnormalities. For example, umbilical proximate cord insertion is higher for multiple pregnancies.
Smoking Cigarettes
Smoking cigarettes during pregnancy increases the risk of placenta previa. Placenta previa increases the risk of Vasa Previa and placental complications like a placental abruption.
Previous C-section or Uterine Surgery

The risk of placenta previa in pregnancy after a C-section is approximately six times higher than after a vaginal delivery. Placenta previa and severe postpartum hemorrhage also frequently follow a history of uterine surgical complications.
Doctors should identify a mother as having a high-risk pregnancy when she has one or more of these risk factors. They must carefully watch for these risks during routine prenatal testing appointments and plan for her labor accordingly.
What Are Vasa Previa Symptoms?
Symptoms of Vasa Previa are typically not noticeable until a mother begins to go into labor. When the membranes rupture, women may experience painless vaginal bleeding that is dark in color. The blood may be darker than is typical because the baby's blood does not have as much oxygen as the mother’s blood. Another common symptom of Vasa Previa is the baby's heart rate, which may be slower. If you notice any bleeding during pregnancy, you should see your healthcare provider immediately.
How is Vasa Previa Diagnosed?

While doctors can identify vasa previa during prenatal testing, symptoms don’t often appear until the mother goes into labor.
Bleeding During Pregnancy
When the membranes rupture, she may experience painless vaginal bleeding that is dark in color. The blood may be darker because the baby's blood does not have as much oxygen as the mother’s blood.
Doctors should perform a transvaginal ultrasound whenever the mother presents with bleeding or any other risk factors. If a mother notices any bleeding during pregnancy, she should alert her healthcare provider immediately.
About Bleeding During Pregnancy
Non-reassuring Fetal Heart Rates

Another common symptom of vasa previa is a slower fetal heart rate, known as bradycardia. This can be a sign of oxygen deprivation and fetal distress.
The baby’s heart rate will react if they suffer from severe blood loss due to compressed or ruptured blood vessels. Other signs on the heart rate monitor may include late decelerations and low/absent variability.
Doctors must carefully watch the baby’s heart rates during labor and delivery to know when to intervene.
When medical professionals fail to notice signs of vasa previa, it may count as medical malpractice. A specialized birth injury lawyer can review medical charts to determine if professionals missed the signs and failed to act.
How to Diagnose Vasa Previa?

An obstetrician or maternal-fetal medicine specialist will typically diagnose vasa previa during a prenatal testing ultrasound. This can help them detect certain placental abnormalities or an irregular fetal heartbeat. The doctor will use a Transvaginal Ultrasound Imaging Device to conduct the ultrasonography. The device inserts into the mother’s vagina to examine her pelvic area, uterus, ovaries, cervix, and fallopian tubes.
Doctors may also use Doppler Color Flow Mapping to trace the umbilical cord to the placental end or uterine wall.
If medical professionals fail to diagnose vasa previa during pregnancy, they may discover it once the mother goes into labor. They should perform an emergency C-section if any of the following complications occur:
- Preterm labor
- Abnormal fetal heart rate patterns and other signs of fetal distress
- Premature rupture of membranes (PROM)
- Sudden and severe vaginal bleeding after the membranes rupture
If a doctor fails to recognize this condition, the fetal vessels will rupture along with the amniotic sac. The mother or her child may need an emergency blood transfusion.
Whenever an expecting mother bleeds at the time of membrane rupture, her healthcare professional should suspect she has vasa previa. An emergency C-section delivery must happen immediately to prevent major damage if the infant's heart is non-reassuring. If they need a blood transfusion after a C-section, the medical team overseeing the delivery should quickly order blood products.
What Are the Consequences of Vasa Previa?
As a result of undiagnosed vasa previa, the newborn may suffer from disabilities like cerebral palsy or Hypoxic ischemic encephalopathy. This is because the compressed blood vessels create an oxygen deficiency in the baby’s blood, which can cause brain injuries.
Perinatal asphyxia can lead to brain damage at birth that leads to the following symptoms and conditions later in childhood:
- Cerebral palsy (CP)
- Seizure disorders
- Permanent brain damage
- Intellectual and developmental delays
- Stillbirth

To improve their condition, children with these disorders will require years of physical, speech, and occupational therapies. They may also require assistive equipment and devices like wheelchairs, specialized beds, and communication devices. The cost of this equipment can sometimes place a taxing financial and emotional burden upon the family.
The best outcomes after vasa previa occur when doctors catch the condition early in the mother’s pregnancy. An obstetrician can detect the complication as early as 18 weeks using a transvaginal ultrasound
How to Treat Vasa Previa?
There is no cure or immediate remedy to eliminate vasa previa. The baby's best chances for avoiding serious birth injuries happen when doctors identify the condition early. As the pregnancy progresses toward full term, the goal of treatment is to closely monitor the mother and her baby.
After diagnosis, the mother’s healthcare provider may schedule nonstress tests twice a week, starting between 28 and 32 weeks. Between 30 and 32 weeks, the provider may recommend early hospital admission for closer monitoring leading up to delivery.
Due to the increased risk of premature labor, doctors should prescribe a steroid called betamethasone between 28-32 weeks gestation. This is a medication that can help the infant's lungs and other organs mature.
Following a vasa previa diagnosis, your healthcare provider should offer you regular follow-up ultrasounds and plan for an early C-section. A physician may schedule the C-section between 34 and 37 weeks. However, delivery can sometimes be earlier if vasa previa puts the mother or baby in imminent danger.
In preparation for a C-section delivery, the doctor may prescribe a shot of corticosteroids to help the pain. If the mother’s membranes rupture early or her baby is in fetal distress, she may require an emergency C-section.
For a successful delivery, medical professionals must carefully craft a pregnancy plan and follow through on it to avoid injury.
Can Vasa Previa Resolve Itself?
Yes, vasa previa can sometimes resolve itself. One study found that 39% of cases of vasa previa resolved on its own. However, the condition typically persists in most cases and puts blood vessels at risk of compression or rupturing.
Even in cases where vasa previa resolves on its own, doctors must still classify the mother’s pregnancy as high risk. They should continue to carefully monitor her condition with follow-up prenatal testing appointments and continued nonstress tests.
Did Doctors Mishandle My Pregnancy Complications?

Uncaught vasa previa can complicate delivery and cause blood loss so severe that it puts the baby’s life at risk. Birth injury negligence, like delaying a C-section or attempting vaginal birth anyway, increases the baby’s risk for injury and death.
If a family believes medical negligence worsened a mother’s labor and delivery, legal support may be an option. A specialized birth injury attorney can review the medical records and circumstances to assess whether a claim exists.
Families who have experienced the effects of birth injuries from negligent medical care deserve to know whether they were avoidable. Our top rated birth injury lawyers will help you find those answers and obtain the necessary funds to secure treatment.
Our National Birth Injury team will thoroughly investigate the facts, holding responsible parties accountable by pursuing medical malpractice claims.
What is the Statute of Limitations in a Birth Injury Lawsuit?

A statute of limitations (SOL) is a law that sets a time limit on how long an injured person has to file a lawsuit after an accident. It is essential to understand that statutes of limitations vary based on the case and the state where you file. For instance, the deadline for birth injury claims is typically different from other claims, such as injury to private property.
Generally, the clock starts ticking on the date the injury occurred. However, there are exceptions to this rule. In some cases, the statute of limitations starts when a person discovers or reasonably should have discovered an injury. When dealing with government agencies, SOLs can become even more complex.
For example, if the party that injured you was:
- A federal employee
- Employed by a military hospital, Veterans Administration facility, or a federally funded medical entity
You may need to file a birth injury claim under the Federal Tort Claims Act (FTCA). In FTCA cases, claimants must go through certain administrative procedures before filing a lawsuit. In some states, you may have less time to give notice if:
- The negligent party was a local or state government hospital
- The doctors and medical providers are employees of a governmental entity
If you file your case outside of the statute of limitations, the court will typically dismiss it. This means you will not be eligible to recover compensation for you or your child’s injuries.
Determining when a statute of limitations begins on your case can be tricky. If you are considering pursuing compensation for a birth injury, contact an attorney as soon as possible.
How Can Our Birth Injury Attorneys Help?

Vasa previa poses a relatively low risk to the baby when doctors identify it before labor. However, it takes an expert review of the facts of your birth to determine whether medical professionals made preventable errors.
Our Process
Our team of specialized birth injury attorneys, nurses and paraprofessionals works to answer these questions and seek compensation. We use our detailed medical negligence case review process to assess your potential birth injury case.
We start by learning more about your pregnancy by gathering records to determine what happened during and after your delivery. This includes evaluating the fetal heart rate strips during labor and the time it took to perform an emergency C-section.
We will call in skilled medical experts who review your records and provide insight into where medical professionals went wrong. If we feel medical negligence caused your baby’s birth injuries or fetal demise, we meet with you to discuss further.
At no point in our legal intake process will we ask you to pay anything. The medical review of your case and the consultation are free. We only receive payment once you do. The sooner you reach out, the sooner we can investigate your case and gather the evidence to support your claim.
We work on a contingency fee basis, meaning you will not pay any legal fees until we win your case. We do not purse any medical malpractice cases unless we fully believe we can win.
Contact us today to schedule your free consultation by calling our toll-free line at (888) 987-0005. You can also reach us by filling out our online request form.
National Birth Injury Law
Our National Birth Injury Attorneys, nurses, and support staff understand that parents of children with birth injuries feel overwhelmed. So, every client has the attention and support of a team of trained, compassionate professionals. But we don’t just offer compassion.
We offer a process to help you discover whether your child’s birth injury, HIE, cerebral palsy or brain injury at birth was caused by medical malpractice.
Call our offices today at (888) 987-0005 for experienced assistance in a free consultation.
Quick Links
Testimonials
- Lyric C. I feel like our voice was heard in a sense of what can possibly go wrong in a delivery and finding us answers. I feel with our settlement, we are now in a comfortable position to provide for our son.
- Lyssa L. They are not just people that say “hey let's get you money and let's go” The law firm was very thorough with us. It was awesome. I don't want to cry, because I think about and it's amazing that they were able to help me and that we were able to help my son and get the story out there.
- Jay C. Throughout the process, one thing was clear to us, the ultimate interest of our child was the utmost concern of Max and his team and as parents navigating a situation like that, that was refreshing to know we had them firmly on our side. I highly recommend them.
Popular Cities
- ★ Dallas Birth Injury
- ★ Houston Birth Injury
- ★ Atlanta Birth Injury
- ★ Chicago Birth Injury
- ★ Philadelphia Birth Injury
Locations
★ Dallas
11551 Forest Central Drive, Ste. 300
Dallas, TX 75243
★ Houston
12929 Gulf Freeway, Ste. 111
Houston, TX 77034